Nursing Diagnosis, Intervention for Cellulitis-Student Guide
Introduction
Cellulitis is a condition that can occur in any part of the body. The most common areas are the legs, arms, and face. It usually starts with redness and then progresses to skin swelling, which is warm to the touch. This blog will provide you with information on what cellulitis is, nursing diagnosis, care plan, and interventions for this condition.
Medical practitioners should know the symptoms to know when to refer patients for medical care or prescribe antibiotics if needed. It can lead to more severe complications such as necrotizing fasciitis (a life-threatening bacterial infection). As you read this blog, keep in mind that our top nursing writers are ready to help in case you get you get stuck with your assignment. All you need to do is place an order with us!
Disclaimer: The information presented in this article is not medical advice; it is meant to act as a quick guide to nursing students, for learning purposes only, and should not be applied without an approved physician’s consent. Please consult a registered doctor in case you’re looking for medical advice.
What is Cellulitis?
Cellulitis is a skin infection that causes redness and swelling of an affected area. It occurs when bacteria enter the skin through a break in the outer layer the skin. The cellulitis infection is more common in people with weakened immune systems, such as the elderly or those with diabetes.
What Are the Causes of Cellulitis?
Cellulitis can be caused by bacteria, viruses, or fungi. It usually starts as an inflammatory process and progresses to necrosis of the underlying tissues in the body. The most common areas affected are the lower extremities, such as the feet and legs.
Cellulitis usually occurs secondary to a break in skin integrity. Minor trauma can cause small breaks in the skin that allow for bacteria and other fluids.
What Are the Risk Factors for Cellulitis?
Cellulitis is more common in people who have poor circulation and sanitation. Infants and the elderly are at a greater risk for cellulitis because of immunosuppression, inflammation, or other underlying conditions.
What Are the Signs and Symptoms of Cellulitis?
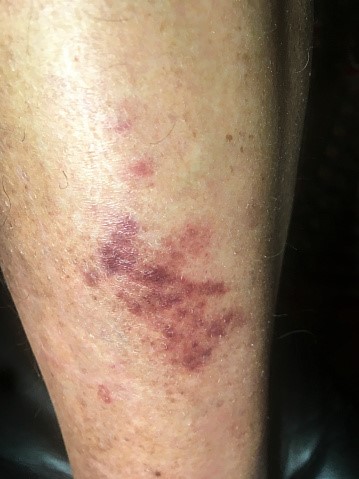
Symptoms can include redness, tenderness, and swelling in an involved area of the body. Skin typically feels hot to the touch. Warmth or pain may occur before skin changes are visible.
Cellulitis can be characterized by one of two different presentations:
-“Erythematous ” occurs when there is redness along with heat and tenderness around the involved area.
-There is often little change in skin color, and there may be no visible discoloration or swelling. This presentation of cellulitis makes it difficult for medical professionals to differentiate from other conditions such as spider bites or insect stings.
What is the Nursing Diagnosis for Cellulitis?


Cellulitis is a nursing diagnosis in which several possible diagnoses should be considered when determining appropriate nursing interventions. The following are some of the nursing diagnoses to consider when caring for a patient with cellulitis:
Tissue integrity, impaired
Impaired skin integrity is a risk factor for cellulitis. Treatment includes cleansing the skin and decreasing tissue pressure that can further break down the cells or tissues. It is essential to assess broken or damaged skin before starting treatment so it doesn’t worsen.
Disturbed sensory perception
Sensory change is a vital sign of cellulitis, and it can occur quickly due to the increased blood flow in an affected area. Identifying changes in sensation will alert medical personnel that care needs to be taken when checking the swollen area or applying pressure.
Pain, acute
Identification of the pain caused by the inflammation in the skin can lead to a better understanding of all body systems. Pain-related cellulitis could affect blood pressure, pulse rate, and systemic levels of medications. Medical professionals need to be aware of any complications that may occur while treating a patient with cellulitis.
Impaired gas exchange secondary to inflammation/infection-
Due to the location of cellulitis around the extremities, there may be impaired gas exchange. This can also lead to a decrease in oxygen and an increase in carbon dioxide levels that healthcare professionals will need to monitor.
What Are the Nursing Interventions for Cellulitis?
Treatment is done by eliminating the source of infection, draining and treating the wound.
-Ensure that the patient is physically comfortable and taking steps to prevent more problems from occurring.
-Making sure the patient is receiving adequate nutrition and hydration.
Ensure patients are getting plenty of rest followed by physical therapy exercises to prevent complications with their blood circulation in the area treated.
Other Nursing Interventions:
* Administer antibiotics intravenously for 7 – 14 days
* Provide emergency care for cellulitis that involves surgery or amputation
* Administer antibiotics orally for 2 – 3 weeks after the wound has healed.
Cellulitis is caused by multiple things such as compromised immune systems, hematomas, and other infections in the area being treated. When treating someone with cellulitis, the essential thing to do is to restore proper blood circulation to the tissue that is causing the damage. Ensure also that they are keeping their body healthy during that time.
Have patients are in an area where they can be monitored 24/7 for any signs of infection or complications. Cellulitis can spread fast. Once it gets into the bloodstream, it can travel to other parts of the body and cause damage to other organs.
If you see someone with this condition, you should call the medical or nurse personnel immediately and let them know what is going on to get that person care as soon as possible.
You can also check interventions for GERD.
How Can You Prevent Cellulitis?
There are a few things that you can do to reduce your chances of contracting cellulitis.
-Stay out of warm pools or hot tubs- places where bacteria and other contaminants tend to thrive.
-Bathe in lukewarm water, and wash thoroughly.
-Do not share towels with others since the spread of germs happens easiest through direct skin-to-skin contact.
Cellulitis is a severe bacterial skin infection that requires prompt treatment to avoid further complications. If patients experience any of the symptoms of cellulitis, they must seek medical attention from their primary care physician or an infectious disease specialist as soon as possible to get the proper treatment.


What Are the Goals of Treatment for Cellulitis?
The goals of treatment are: To destroy causing organism and remove infected tissue. Management is supportive; this means taking care of the client’s needs. This includes relieving pain, controlling infection, supporting the cardiovascular system, and restoring normal skin color and texture by removing dead tissue.
Nursing Care Plan for Cellulitis
Nursing care plans focus on the patients’ needs and goals. The nurse must assess each patient to form a comprehensive nursing diagnosis, create a plan of care that addresses all factors contributing to the illness, administer treatment based on the individualized plan of care and evaluate whether or not the nursing process was successful.
You may check our other comprehensive care plans for Acute Renal Failure
Outpatient Management of Cellulitis
The goal of outpatient management is to improve the wound through debridement and maintain skin integrity until healing is achieved. Provide wound care, including daily dressing changes and cleansing.
-Discuss pain relief options with the patient, such as medications or a nerve block that decreases the amount of pain felt by the patient.
-Provide Education regarding what to do if cellulitis should return or flare up again while in the hospital or at home after being discharged.
Interventions/Strategies for Cellulitis
The following interventions will be used to care for the patients: antibiotic treatment, pain management, assessment of complications, and monitoring skin integrity.
Implementation/Evaluation of Interventions for Cellulitis
Interventions that will be implemented include patient comfort measures such as; maintaining normal body temperature and proper hydration, monitoring vital signs, and skin integrity. The nurse will closely monitor the patient’s progress through physical assessment and evaluation. If the cellulitis is not improving after 24 hours of antibiotic treatment, hospitalization may be necessary to ensure that the infection clears up completely within 72 hours.
Continuous pain management will be implemented to help prevent any unnecessary complications from occurring and ensure the patient’s overall comfort. This includes giving medication as needed for pain, taking vital signs, and providing emotional support.
As a nurse, you may want to check our list of nursing leadership styles to better prepare you to be a nurse leader in your field.
Conclusion
Cellulitis is a prevalent infection caused by bacteria. It can occur on the skin or deep tissue, and if not treated properly, it can have serious consequences, including possible amputation of a limb. Cellulitis occurs most often in patients with diabetes, cancer, or those who are immunocompromised. Nursing care plans will focus on providing proper pain management, antibiotics, and evaluating skin integrity.
Lastly, you can also our check other articles on nursing metaparadigms to increase your knowledge on the nursing philosophy, or our lists of topics in nursing/psychology to make it easier to select a topic for your upcoming essay/research paper. Also, in case you prefer our writers to handle your assignment due to reasons such as a busy schedule, then press the “Write my Nursing Essay” button below and follow the simple steps.